General Information
1. Overview This guidance aims to outline the labelling and packaging requirements for medicinal products intended for human use, following the agreement of the Windsor Framework. It should be used alongside the existing guidance for wholesale dealers and manufacturers. The Windsor Framework establishes long-term arrangements for the distribution of medicines in Northern Ireland. It ensures that medicines can be approved and licensed throughout the UK by the Medicines and Healthcare products Reg...
What Manufacturers and Wholesalers Should Know About MHRA Compliance and the Windsor Framework?
This essential guidance is tailored for manufacturers and wholesale dealers authorized by the Medicines and Healthcare products Regulatory Agency (MHRA). It serves as a comprehensive resource for Qualified Persons (QPs), Responsible Persons (RPs), and Responsible Persons for Import (RPis) to effectively implement the Windsor Framework’s new arrangements for human medicines. Key Responsibilities for Marketing Authorization Holders (MAHs) Marketing Authorization Holders must communicate any chan...
UK-Wide Licensing for Human Medicines
1. Overview This guideline gives information on how the Windsor Framework will be implemented in the UK regarding the licensing of medications for human use. The Medicines and Healthcare Products Regulatory Agency (MHRA) will license medications throughout the United Kingdom starting on January 1, 2025. The Human Medicines Regulations 2012 legislation, as amended by the Human Medicines (Amendments relating to the Windsor Framework) Regulations 2024, and other pertinent...
OMC Medical to Showcase Global Market Access Solutions at KIMES 2024
Book time with Gayathri Ganesan: KIMES Exhibition OMC Medical Set to Attend KIMES, Invites Participants to Meet at UK Pavilion for Uninterrupted Market Access Solutions SEOUL, SOUTH KOREA – February 21, 2024 – OMC Medical, a leading provider of regulatory support and market access solutions for medical device, cosmetics, and pharmaceutical manufacturers, announces its participation in the Korea International Medical & Hospital Equipment Show (KIMES) from March 1...
Global ISO Requirements
What is ISO? ISO – International Organization for Standardization, is the international, non-governmental body for drafting and establishing technical and non-technical standards. These standards are developed by different committees within the International Organization for Standardization. Having around 165 member states, with one representative from each, International Organization for Standardization is a global entity catering to the needs of industry requirements. Are ISO standards impor...
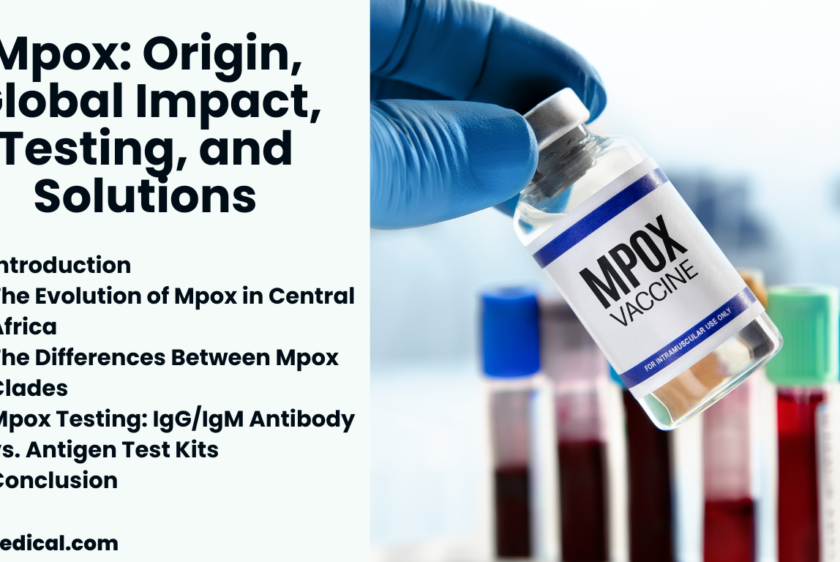
Mpox: Origin, Global Impact, Testing, and Solutions
Mpox, formerly known as monkeypox, is a viral zoonotic disease that has rapidly emerged as a global health concern. The mpox virus, a member of the Orthopoxvirus genus, was first identified in humans in the Democratic Republic of the Congo (DRC) in 1970. For decades, the disease was mostly confined to Central and West Africa, where it remained endemic. However, beginning in the spring of 2022, mpox began spreading to countries outside of Africa, regions that had rarely seen cases in the past. Si...
Product Liability Insurance for Medical devices
Medical devices are subject to product defects. These product defects arise due to design, manufacturing or even a failed instruction for use of a product. These defects can cause risks to patients, who in turn can sue the manufacturer for the damages caused. As medical device manufacturers, it is imperative to choose insurance that best covers themselves as well as their affiliates. Product liability was brought in place to ensure that potentially unsafe products are discouraged from being plac...
Establish a Medical Device Startup Company
Introduction: Medical device startups play an essential role in revolutionizing patient care and improving quality of life. If you share our passion for innovation, starting a medical device company could prove rewarding yet challenging – this article offers comprehensive guidance to help get one started. Tips to start a Medical Device Startup Company 1. Brainstorm an Engaging Idea: Every successful medical device startup begins with an original idea. Start by researching the healthcare in...
Definition of a Medical Device around the global market
What is a Medical Device? The simplest definition of a medical device is a product used for treatment except for medicines. It is imperative to understand if the product classifies as a medical device and apply the regulations after defining it properly. An essential aspect of defining a medical device is its intended use. Intended use is the purpose of the device specified by the manufacturer. In this article, we have brought up the definition of “medical device” for a few major countries....